This article is a repost which originally appeared on Fatherly
Edited for content
Eric developed erectile dysfunction after he started taking the medication he needed to in order to manage symptoms of bipolar disorder. Far more concerned with his mental health than sex life, it took him a while to realize it was a problem. When he did, he thought it was only impacting his relationship with his wife. Then, like a cruel and flaccid Whac-a-Mole game, it started popping up in other places. It impacted his sleep, affected his appetite, and killed his motivation at the gym. Finally, it met him at work. Eric manages a substance abuse recovery facility and has the kind of mentally intense job that people tend to bring home with them. But when his ED started causing problems, the opposite happened — he unintentionally started to bring the stress of his home life into work. With less energy and competitive drive, he struggled to be present and available for his clients when he felt so vulnerable himself.
“It’s really hard to support others when you’re feeling vulnerable,” says Eric (he asked that his real name be held). “We at the center often speak openly and honestly, but erectile dysfunction (ED) is not something I bring up during group sessions. That is such an intimate detail might cloud how clients view me.“
At 36-year-old, Eric may seem young, but he represents the new face of ED. More men in their thirties and forties are developing ED, although the reasons for the uptick are not entirely clear. Whether it’s a side effect of psychotropic medications or other lifestyle factors like smoking and obesity, the fact is, ED is on the rise for younger men, and the costs incurred are just now being calculated. The clearest impacts are economic. Men with ED take more sick days and are generally less productive at work all around, compared to men who do not struggle sexually. Conservative estimates suggest that treatment costs upwards of $3 million in healthcare costs in the U.S. alone, but studies in America have not accounted for the loss of work. Studies in the UK suggest that ED more accurately costs $67.71 million annually when productivity losses are figured in. Adjusted for a larger population in the U.S. amounts to over $330 million. This is a very rough estimate that does not account for cultural differences, but it still likely adds up to a lot of dollars, a lot of dysfunctional dicks, and a lot of other, unknown costs.
“The unseen element of cost is the psychological toll that erectile dysfunction takes on men and their partners and their families,” says urologist Dr. Judson Brandeis. “ED causes depression which decreases productivity at work. It also increases stress on marriages, relationships and families, the cost of which is massive.” How massive? Brandeis estimates the economic cost of ED is well over $5 billion.
And yet, on the other side of ED is a large and burgeoning cross-section of the pharmaceutical industry pedaling generally effective short-term drug solutions like Viagra to older and younger men alike. The global ED drug market was valued at $4.82 billion in 2017 and is projected to grow to $7.10 by the end of 2024. Experts attribute much of this growth to younger men with chronic conditions such as diabetes, cardiovascular disease, neurogenic diseases, and like Eric, psychological disorders, causing an uptick in sexual dysfunction diagnosis. Clearly, ED costs some men money, while it makes others a shit load of it. But the economic impact of ED is farther-reaching than the billions of dollars that surround the drug industry. The function of nearly half the penises in the world is inextricably linked to global economics. Call it the curved economy of dysfunctional dicks. Like it or not, it may impact us all.
🍆 💸 🍆 💸
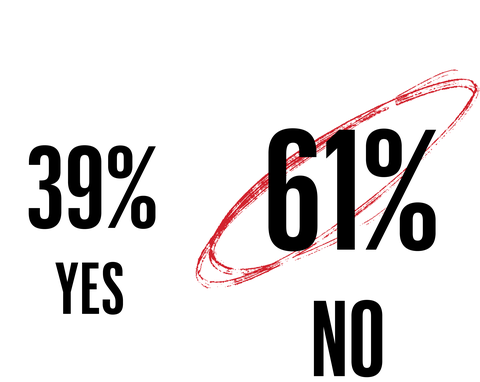
In the past, the most common cause of erectile dysfunction was getting old. As people age, cells in their heart muscle degenerate, valves that control blood flow become thicker and stiffer, and circulation generally slow. Heart health declines, therefore erection health does too, so it has always made medical sense why this would be an issue for retired men in their seventies, rather than men who make up 66 percent of the workforce. However, ED is diagnosed mostly primarily based on patient reports, meaning it’s an honor system, and that’s how a lot of secondary ED diagnoses in younger men are made. Secondary ED, or mild to moderate ED, affects roughly 10 percent of men per decade of life, meaning 30 percent of men in their thirties, 40 percent of men in their forties, 50 percent of men in their fifties, and so on.
Erections depend on blood flow and are inescapably linked with cardiovascular health, so when younger men are unhealthy, they’re more likely to experience ED. In the past, lost productivity at work has been linked to those health problems, and ED was just considered another symptom of an unhealthy lifestyle. A recent study of 52,697 men indicates there may be more to it. Researchers analyzed data from the 2015 and 2016 National Health and Wellness Surveys, which included men ages 40 to 70 from Brazil, China, France, Germany, Italy, Spain, the UK and the U.S. who experienced some form of erectile dysfunction within the past six months of the study. While there was an expected correlation between ED and other health problems like hypertension, dyslipidemia, diabetes, and depression, when scientists controlled for this, men with ED were still worse at their jobs compared to men who felt fine about their sexual performance. Men who experienced symptoms missed more work (7.1 percent compared to 3.2 percent), went to work sick more often (22.5 percent compared to 10.1 percent), experienced greater levels of productivity impairment (24.8 percent compared to 11.2 percent), and scored lower on tests that measure overall mental and physical performance.
“It’s destructive in a workplace situation because men are competing over things that actually have nothing to do with their productivity. Your masculinity being threatened makes you less productive.”
If men’s physical health wasn’t the reason they were struggling at work, then there is something about their professional prowess that is connected to their sexual one. Unsurprisingly, experts suspect a person’s views of masculinity may be responsible for this. Research shows men who cannot perform sexually report a diminished sense of being a man, increased depression, decreased self-worth, embarrassment, and fear of being stigmatized, and the more they believe in traditional masculine norms, the worse they feel as a result of ED.
“This can lower their self-esteem and motivation, even causing physical symptoms such as headaches and lowered immunity,” couples therapist Elisabeth Goldberg explains. When ED goes untreated some men end up feeling worthless. “This is a serious risk factor for depression, leading to missed work days, inability to stick to deadlines, and anger management difficulties with coworkers.”
In the workplace, economist and author Marina Adshade thinks this low self-esteem can take a different turn. Rather than being demotivated by their ED, men become aggressive — in a sense motivated to make up for what they perceive as a masculine failure with a ratcheted-up sense of (usually male on male) competition in the workplace. (catacombepriscilla.com)
“It’s destructive in a workplace situation because men are competing over things that actually have nothing to do with their productivity,” says Adshade. This manifests in ways that may sound familiar: Not being willing to ask for help, not being able to work as part of a team, and not being able to negotiate and compromise. “In the modern workplace, these are real assets. If those are compromised because your masculinity is being threatened, it would make you less productive.”
🍆 💸 💸 🍆
It’s impossible to entirely separate men’s health from erectile dysfunction. Even when studies control for a number of health conditions that cause ED, they do not rule out the possibility that smoking, drinking too much, gaining weight, and being generally unhealthy contributed to missed days and lost productivity for men who did not have diagnosable illnesses.
“It’s a chicken or the egg thing,” says urologist Dr. Jamin Brahmbhatt. “Is it the lifestyle choices that lead to erectile dysfunction or is it erectile dysfunction that lead to the lifestyle choices?” This is a question that may have unsatisfying answers. If lifestyle factors cause ED, it could take years to course-correct — losing weight, quitting smoking, getting back on track health-wise.
Why wait when you can take a little blue pill? While men patiently address varying degrees of underlying health issues, drugs like Viagra represent the closest thing to a catchall solution to a widespread problem. The very success of Viagra may come from the fact that, pending no pre-existing heart conditions, these medications are a generally effective and low-risk solution in the short-term. Aggressive advertising campaigns and direct to consumer healthcare companies that discreetly deliver erection pills door to door have helped reduce stigma and educate men on their ED treatment options. And when Pfizer lost exclusive rights to making Viagra in 2017, this gave rise to a number of generic options and market competition that brought costs down, making it even more affordable and accessible for consumers. ED drugs are a temporary but very effective workaround while men address other underlying health problems that cause sexual dysfunction. Of course, they come with hidden costs.
Everyone might be better off if guys are just fine with whatever they’re working with, even if it doesn’t work every time.
Ironically, medically-induced erections may lead to infidelity. ED is linked with a significantly higher risk of infidelity for men, because they blame their current partner for their performance issues, instead of underlying health, psychological, or relationship problems. “They turn to someone new in a frantic effort to prove their manliness, and rationalize that if they can perform with someone other than their spouse, then it must be the spouse’s fault,” says Goldberg. When it doesn’t, damage done, men can ignore the obvious and use ED drugs like Viagra to help make this warped reality a reality.
Infidelity has economic consequences. The affair itself costs about $450 a month, or $2,700 an affair total, which lasts about 6 months on average. It doesn’t sound like much, but that doesn’t account for time lost to the affair and, of course, the fact that many affairs lead to divorce. While infidelity does not cause divorce directly, it does remain one of the most commonly cited reasons for splitting, about 37 percent of the time. In Goldberg’s clinical experiences, ED can cause marriage problems that lead to divorce without causing infidelity as well.
The average divorce in the U.S. costs $15,000 per person but can vary depending on how drawn out and contentious it is. Research shows divorced men tend to have higher rates of smoking, substance abuse, depression, and worse health overall following divorce, all of which lead to increased absences and decreased productivity at work, which slows economic growth overall. Other studies estimate that the family income of parents who divorce and stay divorced for at least six years falls up to 45 percent.
🍆 🍆 💸 💸
The various impacts of erectile dysfunction can be boiled down to this: Men have unhealthy expectations for how they should perform sexually. “It’s every day in my office, and you can thank the adult film industry for that,” says Brahmbhatt who admits that he spends more time managing men’s impractical sexual expectations than he does writing prescriptions for Viagra.
In a strange way, this psychology echoes in Adshade’s economic research. In her work she stumbled on a global penis size distribution map, a dataset compiled by a doctoral student to look at how a country’s average penis sizes related to their Gross Domestic Product. Although the findings were not published in a peer-reviewed journal, they indicated that there was a u-shaped relationship between penis size and economic growth. The slowest growing and least developed countries had both the biggest and smallest penis sizes on average, but the fastest-growing economies had average ones. Adshade suspects that this was because these were the men who had less to prove in terms of their masculinity, and lead more productive, economically rich lives as a result. While this does not speak to erectile dysfunction directly, it says everything about the economic impact of how men feel about their dicks. Men don’t need to have the biggest or best penises in the world to succeed — in fact, that may be bad for the economy too. But everyone might be better off if guys are just fine with whatever they’re working with, even if it doesn’t work every time.
“ED causes depression which decreases productivity at work. It also increases stress on marriages, relationships and families, the cost of which is massive.”
“It really comes down to how men measure their self-worth,” Adshade says. “Men tend to measure their self-worth by their ability to not only perform sexually but please their partner,” Goldberg adds. “Low-self worth has major consequences”
For Eric, a man who is deep in erectile dysfunction and working on finding a way out, this is easier said than done. For him, Viagra has not been the quick fix it can be for some and he’s working with a urologist to figure out a solution without disrupting his medication regimen. He’s doing pretty much everything he’s supposed to, and it’s still not easy.
“Being a newly-single male back on the dating scene, dealing with ED has been tumultuous, to say the least,” he says. “The toll it takes on men’s confidence is quite drastic. It’s almost as if our masculinity is taken away.”